Physiotherapy Hornsby | Pain & Injury Assessment

Physiotherapy in Hornsby
Physiotherapy (often shortened to “physio”) focuses on assessing and managing pain, injuries, and movement problems. Many people seek a physiotherapist in Hornsby when pain is limiting daily tasks, sport, work, or sleep, or when an injury isn’t settling as expected.
Hornsby Health clinicians may support people with a wide range of concerns - from back, neck, and shoulder pain to sports injuries and postural or load-related problems. A physiotherapy plan is typically tailored after an individual assessment, because symptoms can have more than one contributor.
What is physiotherapy? (And when to seek urgent care)
Physiotherapy is a health service that assesses how the body is moving and functioning, identifies likely contributors to symptoms, and helps people manage pain and improve function through education, activity advice, exercise-based rehabilitation, and other evidence-informed approaches.
Physiotherapy in Hornsby is commonly used to help manage:
- Back and neck pain (acute or persistent)
- Shoulder, elbow, wrist, hip, knee, ankle, and foot pain
- Sports and gym-related injuries
- Tendon pain (for example, Achilles or rotator cuff-related pain)
- Work-related strains (where appropriate to the individual situation)
- Stiffness, reduced mobility, or reduced confidence with movement after an injury

Common contributors to pain and injury (plain language)
Pain and injury can be influenced by one or more factors, including:
- A sudden change in load (for example, lifting, a long walk, a new sport, or returning to the gym)
- Repetitive tasks at work or home
- Reduced strength, endurance, or control around a joint
- Limited mobility or sensitivity in tissues
- Poor sleep, stress, or reduced recovery capacity (which can affect pain sensitivity)
- Previous injuries or long periods of reduced activity
Not all pain means “damage,” and not all tissue changes on imaging explain symptoms. A physio assessment often helps clarify what’s most relevant for the person in front of the clinician.
General red flags (seek urgent medical advice)
Physiotherapy is not a substitute for emergency care. People should seek urgent medical attention (call 000 or attend an Emergency Department) or contact their GP promptly if they have symptoms such as:
- Chest pain, shortness of breath, fainting, or symptoms suggestive of stroke
- Severe, worsening pain after a significant fall, crash, or trauma
- New numbness in the groin/saddle area, new bladder or bowel changes, or rapidly worsening leg weakness
- Fever, unexplained weight loss, night sweats, or feeling very unwell alongside new severe pain
- Night pain that is severe and unrelenting, especially if it doesn’t change with position
- Suspected fracture, dislocation, or infection
If uncertain, it is safer to seek medical assessment first.
How Hornsby Health clinicians assess pain and injury
A physiotherapy assessment generally aims to understand what is happening, why it may be happening, and what can be done to move forward safely. At Hornsby Health, our clinicians may also work alongside chiropractic and exercise physiology services depending on the person’s needs, preferences, and goals.
1) History: understanding the story
A physio will usually ask about:
- Where symptoms are felt, how they began, and how they behave over the day
- What makes symptoms better or worse (for example, sitting, bending, walking, lifting)
- Past injuries, general health factors, activity levels, and sleep
- Work demands and recreational goals
- Current self-management strategies and what has or hasn’t helped so far
This information helps guide the physical examination and identify any signs that may need medical referral.
2) Physical examination: movement and function
The physical exam often includes:
- Observing posture and movement patterns relevant to the complaint
- Checking range of motion, strength, and control
- Testing functional tasks (for example, squatting, stepping, lifting mechanics), where appropriate
- Palpation (gentle assessment of tissues) and specific tests to help narrow likely contributors
The goal is not just to “find a sore spot,” but to identify modifiable factors that can be targeted in a plan.
3) Screening and clinical reasoning
Physios commonly screen for:
- Neurological signs (for example, reflexes, sensation, strength changes)
- Red flags suggesting non-musculoskeletal causes of pain
- Factors that can influence recovery (for example, deconditioning, load tolerance, confidence with movement)
Where imaging or further tests are relevant, clinicians may discuss this with the patient and suggest GP review. Many musculoskeletal conditions do not require imaging initially, but this depends on the individual presentation.
4) Shared goals and planning
Hornsby Health clinicians may work with the person to set practical goals such as:
- Reducing pain flare-ups
- Returning to work tasks more comfortably
- Building walking tolerance
- Getting back to sport or gym training
- Improving confidence with lifting, bending, or running
A plan is typically adjusted over time based on response and progress, because recovery is rarely perfectly linear.

Treatment and management options in Hornsby
Physiotherapy management often involves a combination of education, graded exercise, and strategies that support daily function. What is used (and when) depends on the assessment findings, the person’s health history, and what they prefer.
Education and reassurance (without dismissing symptoms)
Many people find it helpful to understand:
- What structures may be involved and what that means (and doesn’t mean)
- How pain can change with stress, fatigue, load, and recovery
- How to stay active safely without pushing into repeated flare-ups
Education is typically paired with a practical plan, not just advice to “rest.”

Activity modification and pacing
For many injuries, it can be helpful to temporarily adjust aggravating activities while keeping the body moving. This might include:
- A short-term change to training volume, intensity, or technique
- Modifying work tasks where feasible
- Breaking up prolonged sitting or standing
- Using pacing strategies to reduce boom–bust cycles (doing too much on good days, then flaring)
Exercise-based rehabilitation (often central)
Exercise is commonly used to improve:
- Strength and capacity (tolerance to load)
- Mobility (where stiffness is relevant)
- Control and coordination
- Conditioning and confidence with movement
Programs are usually progressed gradually. For example, someone with back pain may start with gentle movement and walking tolerance, then build trunk and hip capacity, and later return to heavier lifting or sport-specific training as appropriate.
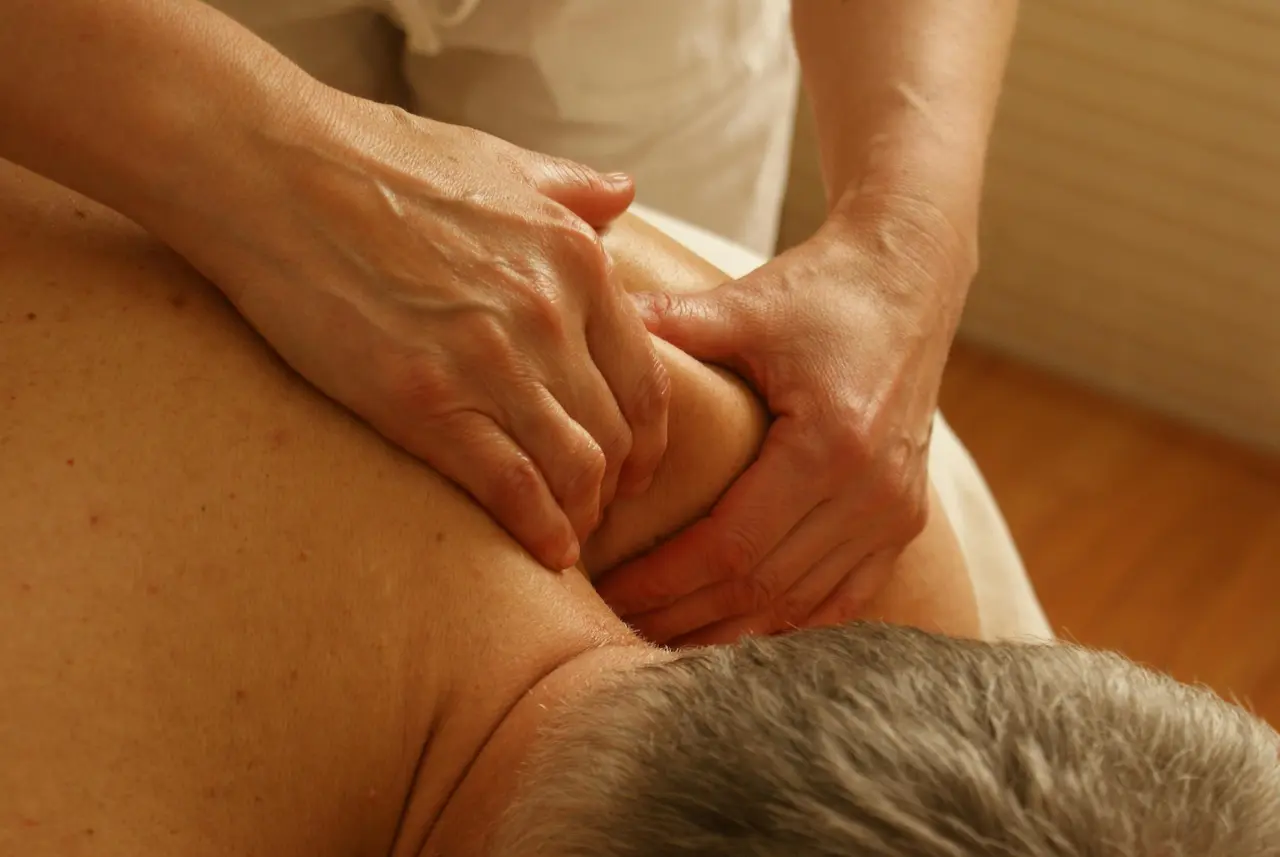
Hands-on options (used selectively)
Some physiotherapy approaches include hands-on care, which may be used to reduce symptoms in the short term and support participation in rehabilitation. This can include techniques such as soft tissue work or joint mobilisation, depending on clinician judgement and patient preference. Hands-on care is typically most useful when paired with active rehab and self-management.
Self-management strategies between visits
A physiotherapist may provide guidance on:
- Home exercises (simple, time-efficient options)
- Heat/ice use where appropriate
- Sleep and recovery habits that may influence pain sensitivity
- Building a sustainable weekly routine for movement
When referral or co-management may be appropriate
Sometimes, the safest and most effective next step involves additional support, such as:
- GP review for medications, imaging decisions, or broader health screening
- Specialist referral when symptoms suggest a more complex condition
- Co-management with exercise physiology for longer-term conditioning or return-to-exercise planning
- Coordination with other providers where relevant and with patient consent
Outcomes vary, and the timeline depends on the condition, overall health, and how the issue responds to management.
Common questions about physiotherapy in Hornsby
Do I need a referral to see a physiotherapist?
In many cases, people can book directly with a physiotherapist. However, some funding pathways or compensable schemes may have different requirements. If unsure, it can help to ask the clinic or check with the relevant insurer or scheme.
How many sessions will I need?
It varies. Some people need only a small number of appointments for assessment, guidance, and a home plan, while others benefit from a longer block of care to build strength and confidence and reduce recurrence. The clinician may discuss a likely plan after the initial assessment and adjust it based on progress.
Will I get exercises?
Many physiotherapy plans include exercises, because building capacity often supports longer-term results. The exercises are usually chosen to match current tolerance and goals, and they can often be completed at home with minimal equipment.
Does physiotherapy help back pain?
Physiotherapy is often used to manage back pain by improving movement confidence, addressing contributing factors (such as load tolerance and conditioning), and supporting a graded return to normal activities. Because back pain has many possible drivers, an individual assessment matters, and results can vary.
Should I rest until the pain is gone?
Complete rest is not always helpful. Many people do better with relative rest (reducing aggravating tasks) while staying active with tolerable movement. A physiotherapist can help identify what is safe to keep doing and what to modify temporarily.
What if my pain keeps coming back?
Recurring pain can have multiple contributors, including load spikes, reduced strength/conditioning, poor recovery, stress, or habits that increase sensitivity. A plan may focus on preventing flare-ups through progressive strengthening, pacing, and strategies that fit real life, not just short-term symptom relief.
Who this may help in Hornsby and nearby suburbs
Physiotherapy may be relevant for people across Hornsby and surrounding areas such as Waitara, Asquith, Wahroonga, Thornleigh, and Mount Colah who want practical support for pain, injury, and movement goals.
Common scenarios include:
- Office and remote workers with neck, shoulder, or upper back pain linked to prolonged sitting and reduced movement variety
- Active people with gym or running injuries, including tendon pain or flare-ups after changing training load
- People with low back pain affecting lifting, gardening, housework, or long drives
- Parents and carers managing aches from lifting, carrying, and repetitive tasks
- People returning to activity after time off due to illness, stress, or reduced fitness
- People with persistent pain who want a structured plan to build confidence and function at a manageable pace
Even when two people have similar symptoms, the best plan can look different depending on health history, goals, and day-to-day demands.
Next steps
If pain or injury is persisting, worsening, or interfering with work, exercise, or sleep, an assessment with a physiotherapist in Hornsby may help clarify what’s going on and what to do next. Our clinicians may discuss suitable management options and help plan a safe, progressive return to the activities that matter.
If symptoms include any red flags (such as significant trauma, severe worsening pain, or new bladder/bowel changes), it is important to seek urgent medical care or GP advice.

Ready to book an appointment with us?
Visit our Online Bookings page where you can see what times are available and book appointments with all our great Physiotherapists, Chiropractors, and Exercise Physiologists in Hornsby. You can also find us and book appointments via HotDoc and HealthEngine.
Rather speak to someone? Simply give us a call on 02 8428 0528 and our friendly receptionists can help you find a time that suits, and answer any questions you might have.
%20(1).svg)
.svg)



